GLP-1 Therapy for Eating Disorder: Understanding the Connection
Glucagon-like peptide-1 (GLP-1) therapy has emerged as a promising treatment for various medical conditions, including diabetes and obesity. However, its impact on eating disorders has sparked a growing conversation in the medical community. As research continues to unravel the complexities of GLP-1 therapy for eating disorders, it is essential to explore the connection between the two and the potential risks and benefits associated with this treatment.
Risks of Eating Disorder Relapse and Misuse
Rapid weight loss and appetite changes caused by GLP-1 drugs can mimic eating disorder symptoms, making it challenging to distinguish treatment effects from relapse. This is particularly concerning for individuals with a history of eating disorders, as GLP-1 therapy may exacerbate underlying issues. Clinicians report that GLP-1 drugs can worsen or hide eating disorders by suppressing hunger cues, potentially undermining recovery strategies like intuitive eating.

This particular example perfectly highlights why Glp-1 Therapy For Eating Disorder is so captivating.
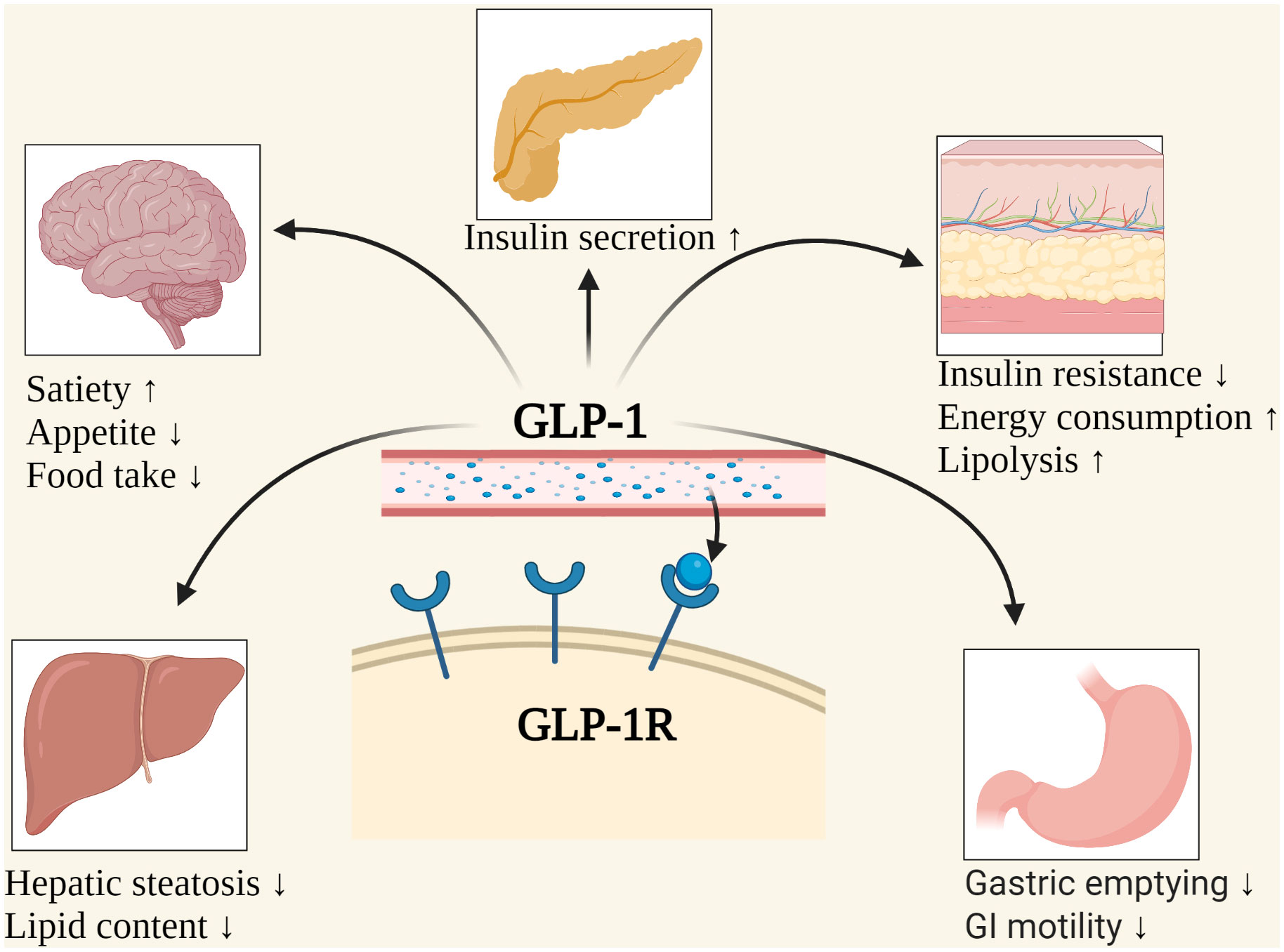
Understanding GLP-1 and Eating Disorders
GLP-1 Therapy and Eating Disorder Treatment
In some cases, GLP-1 therapy may be used in conjunction with behavioral therapy and nutritional counseling for eating disorder treatment. However, this approach requires careful evaluation and monitoring to ensure that the patient is not using the medication as a means to manipulate their weight or appetite. FDA approval exists for liraglutide (Saxenda) specifically for binge eating disorder treatment, highlighting the potential benefits of GLP-1 therapy in this context.

Such details provide a deeper understanding and appreciation for Glp-1 Therapy For Eating Disorder.
Risks and Side Effects of GLP-1 Therapy for Eating Disorders
Clinicians report that GLP-1 drugs can have various side effects, including nausea, vomiting, and diarrhea, which may exacerbate eating disorder symptoms. Additionally, GLP-1 therapy may mask symptoms of restrictive eating disorders, as rapid weight loss, nausea, and reduced appetite are common effects of the medication. This highlights the importance of careful medical monitoring and regular follow-up appointments to ensure that the patient is not developing any adverse effects.
Alternatives to GLP-1 Therapy for Eating Disorders

Such details provide a deeper understanding and appreciation for Glp-1 Therapy For Eating Disorder.
While GLP-1 therapy may be beneficial for some patients with eating disorders, it is not the only option. Behavioral health is an essential consideration before starting GLP-1 medications, and a history of trauma, eating disorders, or other mental health concerns should be carefully evaluated before and during treatment. Alternatives to GLP-1 therapy include cognitive-behavioral therapy, family-based therapy, and other evidence-based treatments for eating disorders.
Conclusion
GLP-1 therapy has emerged as a promising treatment for various medical conditions, including diabetes and obesity. However, its impact on eating disorders is complex and multifaceted, and further research is needed to fully understand the risks and benefits associated with this treatment. As clinicians, patients, and researchers continue to explore the connection between GLP-1 therapy and eating disorders, it is essential to prioritize careful medical monitoring, regular follow-up appointments, and evidence-based treatments to ensure the best possible outcomes for patients with eating disorders.